Blood test predicts dementia in women years before symptoms begin

Study finds biomarker p-tau217 strongly linked to future dementia risk
Researchers from the University of California San Diego and Kaiser Permanente Washington Health Research Institute (KPWHRI) have found that a novel blood-based biomarker can predict a woman’s risk of developing dementia as many as 25 years before symptoms appear. The study, published in JAMA Network Open, shows that higher levels of phosphorylated tau 217 (p-tau217) — a protein linked to the brain changes seen in Alzheimer’s disease — were strongly associated with future mild cognitive impairment and dementia among older women who were cognitively healthy at the start of the study.
“Our study suggests we may be able to identify women at elevated risk for dementia decades before symptoms emerge,” said Aladdin Shadyab, PhD, MPH, first author of the study and UC San Diego associate professor of public health and medicine at the Herbert Wertheim School of Public Health and Human Longevity Science and the School of Medicine. “That kind of long lead time opens the door to earlier prevention strategies and more targeted monitoring, rather than waiting until memory problems are already affecting daily life.”
The findings are based on data from 2,766 participants in the Women’s Health Initiative Memory Study, a large national study that enrolled women ages 65 to 79 in the late 1990s and followed them for up to 25 years. All women were cognitively unimpaired when they entered the study, meaning that no memory or thinking problems had been detected. Blood samples collected at the start of the study were analyzed years later to measure p-tau217, a form of tau protein that reflects early brain changes associated with Alzheimer’s disease.
Over the years of follow-up, researchers identified women who developed memory or thinking problems, including dementia. Those who had higher levels of p-tau217 in their blood at the start of the study were much more likely to develop dementia later in life. In fact, as levels of this biomarker increased, so did dementia risk. Women with the highest p-tau217 levels faced the greatest likelihood of developing dementia over the long term.
However, the researchers also found that the risk of cognitive impairment or dementia associated with higher levels of p-tau217 was not the same for everyone. For example, higher p-tau217 levels were more strongly associated with poorer cognitive outcomes among women who were over age 70 at the start of the study and among those with the APOE4 genetic risk factor for Alzheimer’s disease. The study also found that p-tau217 was more predictive of dementia among women who had been randomized to estrogen plus progestin hormone therapy versus placebo.
“Blood-based biomarkers like p-tau217 are especially promising because they are far less invasive and potentially more accessible than brain imaging or spinal fluid tests,” said senior author Linda McEvoy, PhD, a senior investigator at KPWHRI and professor emeritus at the Herbert Wertheim School of Public Health. “This is important for accelerating research into the factors that affect risk of dementia and for evaluating strategies that may reduce risk.”
Currently, blood-based biomarkers are not recommended for clinical use in people without symptoms of cognitive impairment. The authors noted that additional studies are needed to determine how p-tau217 testing might be used in routine clinical care and whether early identification can meaningfully change outcomes. Future research will also explore how factors such as hormone therapy, genetics, and age-related health conditions interact with plasma p-tau217 over the course of someone’s life to affect dementia risk.
“Ultimately, the goal is not just prediction,” Shadyab added, “but using that knowledge to delay or prevent dementia altogether.”
Read the paper: Plasma phosphorylated tau 217 and incident mild cognitive impairment and dementia in older women, published in JAMA Network Open.
Adapted from a press release provided by University of California San Diego.
Research
Autopsy study links BP drugs to possible brain benefits
Research supports theory that some blood pressure medications may provide extra protection against dementia.
Research
ACT Study contributes to understanding Alzheimer’s disease in brain cells
Mapping the disease at the cellular level identifies possible new treatment targets.
Research
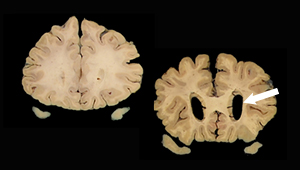
Study evaluates biomarker criteria for Alzheimer’s risk
One-third of people classified as ‘highest risk’ may not develop Alzheimer’s disease, study suggests



