Dementia risk tied to blood sugar level, even with no diabetes
University of Washington–Group Health study in New England Journal of Medicine
Seattle, WA—A joint Group Health–University of Washington (UW) study in the New England Journal of Medicine has found that higher blood sugar levels are associated with higher dementia risk, even among people who do not have diabetes.
Blood sugar levels averaged over a five-year period were associated with rising risks for developing dementia, in this report about more than 2,000 Group Health patients age 65 and older in the Adult Changes in Thought (ACT) study.
For example, in people without diabetes, risk for dementia was 18 percent higher for people with an average glucose level of 115 milligrams per deciliter compared to those with an average glucose level of 100 mg/dl. And in people with diabetes, whose blood sugar levels are generally higher, dementia risk was 40 percent higher for people with an average glucose level of 190 mg/dl compared to those with an average glucose level of 160 mg/dl.
“The most interesting finding was that every incrementally higher glucose level was associated with a higher risk of dementia in people who did not have diabetes,” said first author Paul K. Crane, MD, MPH, an associate professor of medicine at the UW School of Medicine, adjunct associate professor of health services at the UW School of Public Health, and affiliate investigator at Group Health Research Institute. “There was no threshold value for lower glucose values where risk leveled off.”
“One major strength of this research is that it is based on the ACT study, a longitudinal cohort study, where we follow people for many years as they lead their lives,” said senior author Eric B. Larson, MD, MPH, a senior investigator at Group Health Research Institute who also has appointments at the UW Schools of Medicine and Public Health. “We combine information from people’s research visits every other year with data from their visits to Group Health providers whenever they receive care. And this gave us an average of 17 blood sugar measurements per person: very rich data.”
These measurements included blood glucose (some fasting, some not) and glycated hemoglobin (also known as HbA1c). Blood sugar levels rise and fall in peaks and valleys throughout each day, but glycated hemoglobin doesn’t vary as much over short intervals.
Combining glucose and glycated hemoglobin measures into a composite measure required special statistical techniques, which Drs. Crane and Larson’s co-authors Rod Walker, MS, a biostatistician, and Rebecca Hubbard, PhD, an associate investigator, both from Group Health Research Institute, had developed. (Dr. Hubbard is also an affiliate assistant professor of biostatistics at the UW School of Public Health.) These sophisticated statistical models required specialized data on the relationships between glycated hemoglobin and glucose levels, and they used data generated by co-author David M. Nathan, MD, a professor of medicine at Harvard Medical School and director of the Diabetes Center at Massachusetts General Hospital.
So should people try to eat less sugar—or foods with a lower “glycemic index”? Not necessarily, Dr. Crane said: “Your body turns your food into glucose, so your blood sugar levels depend not only on what you eat but also on your individual metabolism: how your body handles your food.” But he does suggest that taking walks couldn’t hurt: The ACT study has previously linked physical activity to later onset and reduced risk of dementia, including Alzheimer’s disease.
Furthermore, Dr. Crane emphasized that these results come from an observational study: “What we found was that people with higher levels of glucose had a higher risk of dementia, on average, than did people with lower levels of glucose,” he said. “While that is interesting and important, we have no data to suggest that people who make changes to lower their glucose improve their dementia risk. Those data would have to come from future studies with different study designs.”
More research is planned to delve into various possible mechanisms for the relationship between blood sugar and dementia. “This work is increasingly relevant,” Dr. Crane said, “because of the worldwide epidemics of dementia, obesity, and diabetes.”
The study was supported by grant U01 AG06781 (Dr. Larson, principal investigator) from the National Institute on Aging of the National Institutes of Health.
Additional co-authors included Ge (Gail) Li, MD, PhD, associate professor of psychiatry and behavioral sciences, Thomas Montine, MD, PhD, professor and chair of pathology, Wayne McCormick, MD, MPH, professor of medicine, all at the UW School of Medicine; Susan McCurry, PhD, research professor in the UW School of Nursing, adjunct research professor of psychiatry and behavioral sciences at the UW School of Medicine, and an affiliate investigator at Group Health Research Institute; Steven Kahn, MB, ChB, professor of medicine at the UW School of Medicine and VA Puget Sound Healthcare System and director of the UW’s Diabetes Research Center; Hui Zheng, PhD, assistant professor at Harvard Medical School and Massachusetts General Hospital; Sebastien Haneuse, PhD, associate professor of biostatistics at Harvard School of Public Health; Suzanne Craft, PhD, professor of gerontology and geriatric medicine at Wake Forest School of Medicine, in Winston-Salem, NC; and James Bowen, MD, of Swedish Neuroscience Institute in Seattle.
Adult Changes in Thought (ACT) study
Begun in 1994, the Adult Changes in Thought (ACT) study is a collaboration between Group Health and the University of Washington. This longitudinal study follows adults age 65 and older to identify risk factors for cognitive decline with aging and related conditions, such as Alzheimer's disease. Men and women with no cognitive impairment are randomly selected and invited to participate. At the time of enrollment, all are Group Health members. Participants visit the Group Health Research Clinic every two years for physical and cognitive assessments. By combining these data with comprehensive medical and pharmacy records and biospecimens collected at the baseline enrollment visits, investigators have established a promising scientific resource for understanding dementia, including Alzheimer's disease. The study continues to follow people still alive from the original enrollment and replaces those who die with new volunteers, keeping study enrollment at about 2,000 people. The ACT study and its predecessor, the UW–Group Health Alzheimer's Disease Patient Registry, have had continuous National Institutes of Health (NIH) funding for 27 years. Like the celebrated Framingham Heart Study, ACT is a longitudinal cohort study of people leading their lives in a community. That means it follows a large group of people at regular intervals over a long time to see what happens to them. A distinguishing feature of ACT is that, because its participants are selected from patients in the Group Health care-delivery system, the study has access to extensive information collected during visits to providers that happen separate from the study.
UW Medicine
The UW Medicine health system includes Harborview Medical Center, Northwest Hospital and Medical Center, Valley Medical Center, UW Medical Center, UW Neighborhood Clinics, UW Physicians, UW School of Medicine, and Airlift Northwest. UW Medicine also shares in the ownership and governance of Children’s University Medical Group and Seattle Cancer Care Alliance, a partnership among UW Medicine, Fred Hutchinson Cancer Research Center, and Seattle Children’s. UW Medicine has major academic and service affiliations with Seattle Children’s, Fred Hutchinson Cancer Research Center, Veterans Affairs Puget Sound Health Care System in Seattle, and the VA Hospital in Boise, Idaho. The UW School of Medicine is the top public institution for biomedical research in funding received from the National Institutes of Health.
About Kaiser Permanente
Kaiser Permanente is committed to helping shape the future of health care. We are recognized as one of America’s leading health care providers and not-for-profit health plans. Founded in 1945, Kaiser Permanente has a mission to provide high-quality, affordable health care services and to improve the health of our members and the communities we serve. We currently serve more than 12.4 million members in eight states and the District of Columbia. Care for members and patients is focused on their total health and guided by their personal Permanente Medical Group physicians, specialists and team of caregivers. Our expert and caring medical teams are empowered and supported by industry-leading technology advances and tools for health promotion, disease prevention, state-of-the-art care delivery and world-class chronic disease management. Kaiser Permanente is dedicated to care innovations, clinical research, health education and the support of community health. For more information, go to: kp.org/share.
Rod L. Walker, MS
Principal Collaborative Biostatistician
Study link:
Media contact
For more on Kaiser Permanente Washington Health Research Institute news, please contact:
Bianca DiJulio
bianca.s.dijulio@kp.org
206-660-8333
After-hours media line: 206-448-4056
ACT study
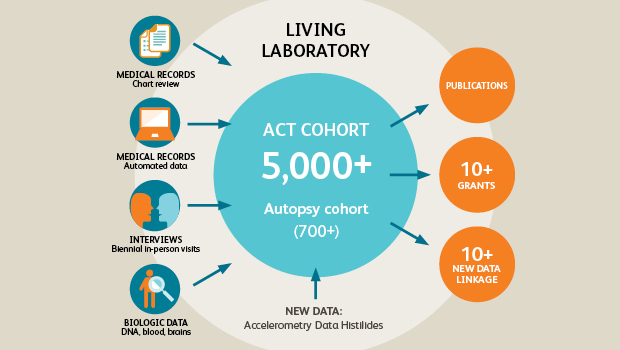
ACT study: Long-running study of aging examines changes in Group Health patients over time
Drs. Larson and Crane co-lead Group Health-University of Washington collaboration learning how to promote healthy aging.


