Improving and advancing mental health care

KPWHRI researchers are contributing to better mental health care for people nationwide
Improving and advancing mental health care is a key goal for researchers at Kaiser Permanente Washington Health Research Institute (KPWHRI). According to data from the National Institute of Mental Health, nearly a quarter of adults and almost half of adolescents in the U.S. were living with a mental illness in 2021. Our researchers are finding ways to improve access to mental health care, reduce disparities, and identify patients who could benefit from support and appropriate treatment before they develop severe symptoms. In recognition of Mental Health Awareness Month, here are some highlights of their current work.
Helping clinicians use suicide risk prediction tools
KPWHRI researchers lead important work in the field of suicide prevention. This includes development of a suicide risk prediction model that performs significantly better than other screening tools, which rely on self-reports from patients. However, the work doesn’t end with model development. In partnership with Kaiser Permanente Washington clinical teams, researchers are working to make sure that the model is integrated into clinical care in a way that considers the needs of its users.
“When the suicide risk prediction algorithm was first put into use at Kaiser Permanente Washington, we found that it wasn’t consistently leading to additional follow-up with patients identified as high risk,” said Julie Richards, PhD, MPH, a senior collaborative scientist at KPWHRI who is leading the implementation project with the institute’s Center for Accelerating Care Transformation (ACT Center).
The results of the pilot led to a redesigned implementation process based on feedback from clinicians about their needs and barriers they reported in using the algorithm data to guide care for their patients. Clinicians expressed concerns about the reliability of the risk prediction model, lack of communication after implementation, and usability issues with the electronic health record.
The research team decided to employ a user-centered design approach that mapped existing workflows for suicide care and brought in clinical stakeholders to talk about challenges and the context in which the tool would be used. Based on that process, they created improved clinical decision tools and workflows, which were implemented in December 2022. In March 2023, a usability survey went out to clinicians, which will provide additional insight and guidance for next steps.
"A model can be extremely accurate, but our real goal is to make sure people get the care they need," said Gregory Simon, MD, a senior investigator at KPWHRI and lead of the Mental Health Research Network. "Following up to make sure this model could be implemented and used to its fullest potential is a crucial part of the work we do."
The model implemented at Kaiser Permanente Washington underwent careful evaluation to ensure that it did not perpetuate existing health disparities. However, some prediction models do not accurately identify high-risk patients from all racial and ethnic groups. Yates Coley, PhD, a biostatistics researcher at the institute, is now working on a project to develop new statistical methods for reducing racial and ethnic disparities in prediction model performance, which will help health systems and research teams improve model evaluation and design.
Catching mental health disorders early
Another algorithm still in development could lead to a clinical tool for predicting the risk of a mental health diagnosis, specifically a diagnosis where a person experiences loss of contact with reality (also known as psychosis). The symptoms of psychosis often appear in young adulthood but can also accompany other diseases or be triggered by stressors or external factors, according to the National Institute of Mental Health. Researchers at KPWHRI are collaborating with Kaiser Permanente Northern California to analyze data from health care visits over a 3-year period using natural language processing.
The researchers hope to identify words and phrases that appear more often for patients who eventually go on to receive a new psychotic-spectrum diagnosis. They will use that data to build a prediction model that, if successful, could be integrated into clinical care, helping clinicians to identify patients at risk of this serious health condition and create opportunities for early intervention.
Guiding earlier care and reducing disparities for youth
Mental illnesses often appear in childhood, but many children do not receive treatment. In 2021, the U.S. Surgeon General issued an advisory on protecting youth mental health, responding to increasing rates of depression and suicidal ideation in youth and the impact of the COVID-19 pandemic on mental health.
Researchers at KPWHRI are testing an intervention to guide earlier access to mental health services for youth with mental health symptoms or concerns. Using a predictive algorithm that draws from data in the electronic health record, they identify patients ages 4 to 12 who have documented symptoms from a recent health care visit but have not started treatment. Study participants in the intervention group will have the option of 6 months of family support from a social worker, including an assessment of the family’s needs and any barriers to mental health services, as well as help scheduling mental health appointments and access to video-based psychotherapy when appropriate. The study will measure whether patients who receive the intervention attend more mental health visits over a 6-month period than those in the control group. The researchers will also compare improvements in mental health symptoms between the 2 groups.
“We hope to show that the navigator intervention increases mental health services use and positive outcomes so that these children go on to maximize their human potential,” said Robert Penfold, PhD, a senior investigator at KPWHRI and lead of the project.
Another project, led by KPWHRI Collaborative Scientist Rosemary Meza, PhD, is exploring the use of peer support to reduce disparities in youth mental health outcomes in Washington state. Peer support is a relationship-based approach where people in recovery draw on their shared lived experience to support patients through their own recovery. In Washington, peer counseling is an approved service through Medicaid, and peer counselors are certified after taking a test and meeting certain requirements.
The research team is conducting a literature review and working with publicly funded community mental health clinics to understand how and why peer support works, and how it is currently implemented at those sites. They will then identify areas for optimization and develop theory-driven models of peer support that can be tested in future studies.
“Peer support has been an important resource in increasing engagement and access to mental health services,” Meza said. “Our team is trying to build on this important resource to expand its reach and impact.”
IMPACT Center

Improving mental health care for youth
A new center will support using evidence-based practices in under-resourced settings such as schools.
mental health
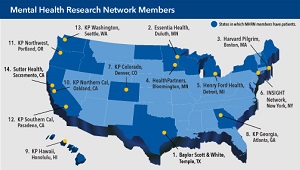
$10 million to expand Mental Health Research Network
NIMH funding will enable the MHRN to conduct larger studies in integrated health systems on topics that matter most.
Healthy Findings Blog

Delivering on the real promise of virtual mental health care
Dr. Gregory Simon tells how telehealth, prompted by COVID-19, shifts care from passive response to active outreach.


